Pharynx
The pharynx is a wide muscular tube extended behind the nasal cavity - mouth cavity & behind the larynx up to the lower border of the cricoid cartilage, from where it is continued as the esophagus
Length of pharynx- 12cm
Pathway for air
Air- Nose- Nasal cavity
|
Posterior nasal apparatus
|
Nasopharynx
Oropharynx
|
Laryngeal inlet
Larynx
|
Below the lower border of the cricoid cartilage
The larynx is continuous as Trachea
Pathway of food
Mouth cavity
|
Oropharynx
Laryngopharynx
Below the lower border of the cricoid cartilage, laryngopharynx is continued as the esophagus.
To sum up as a whole
Nasopharynx(Air)
|
Oropharynx(Air + Food)
|
Larynx (Air) Laryngopharynx (Food)
At the lower border of the cricoid cartilage, corresponding to 6th cervical vertebrae, they continued as
| |
Trachea Oesophagus
Note: Laryngeal inlet bounded on each side by piriform fossa.
Important landmark from cricoid cartilage
Cricoid cartilage correspond to the level of 6th cervical vertebrae
Form the lower border of cricoid cartilage:
- Larynx is continuous below as Trachea
- Laryngopharynx is continued below as esophagus
From the upper border of the thyroid cartilage,
The common carotid artery bifurcated into external and internal carotid artery.
Boundary of pharynx as a whole
Superiorly
Base of the skull, with the basilar part of the occipital bone (in front of the pharyngeal tubercle) & the posterior part of the sphenoid.
Inferiorly
Pharynx is continuous with the esophagus at the lower border of the cricoid cartilage, corresponding to the level of 6th cervical vertebra
Posteriorly
Retropharyngeal space, prevertebral fascia which separates it from the cervical vertebral bodies
Anteriorly
Communicates with:
- Nasal cavity through posterior nasal aperture
- Oral cavity through oropharyngeal isthmus
- Larynx through laryngeal inlet, which is bounded on either side by piriform fossa
Note:
Oropharyngeal isthmus is the junction between the mouth cavity and oropharynx
- Superiorly by soft palate
- Inferior by the posterior part of the tongue
- On each side palatoglossal arches
Nasopharyngeal isthmus:
Junction between nasopharynx and oropharynx
It represents the location where soft palate lies during the swallowing of food so that food doesn’t enter into the nasopharynx.
Communication of pharynx
- Anterosuperiorly - Posterior nasal aperture
- Anterior of middle part - Mouth cavity
- Inferiorly with esophagus
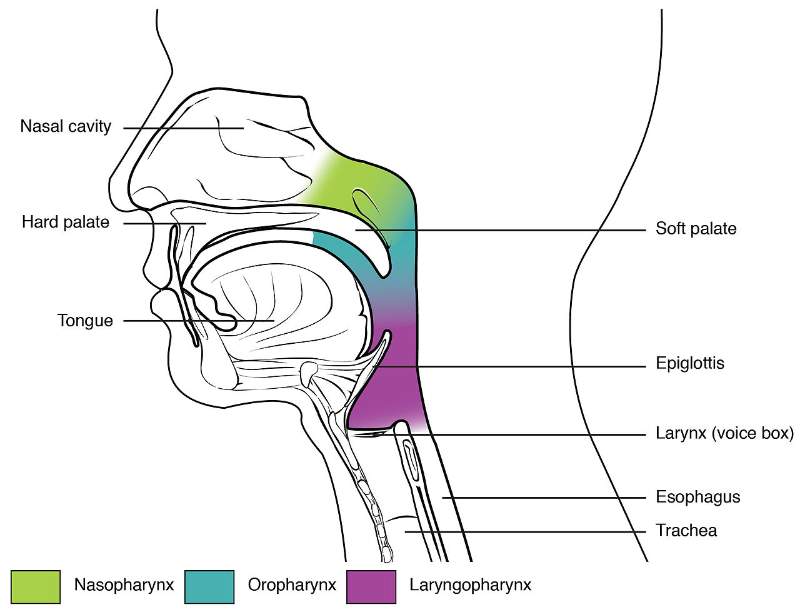
Part of Pharynx
- Nasopharynx
- Oropharynx
- Laryngopharynx
Function
- Nasopharynx: Transmit only air
- Oropharynx: Transmit both air & food
- Laryngopharynx: Transmit food
Lining epithelium
Nasopharynx: respiratory epithelium
Pseudostratified ciliated columnar epithelium
Oropharynx & Laryngopharynx:
Non-keratinized stratified squamous epithelium
Signification of Lateral wall:
Nasopharynx:
There is recess or fossa (slightly depressed fossa) behind the opening of the cartilaginous part of the auditory tube on the lateral wall of the nasopharynx
This is called as Pharyngeal Recess or Fossa of Rosenmuller.
Clinical importance: It is the major common site of origin of nasopharyngeal carcinoma.
Structure of Pharynx:
The wall of the pharynx presents 5 coats from inside to outward
- Mucosa
- Submucosa
- Pharyngobasilar fascia
- Muscular coat
Outer circular layer made of three constrictors
Inner longitudinal muscle layer
5. Buccopharyngeal fascia
Description
Mucous membrane lined by non-keratinized stratified squamous epithelium except nasopharynx which is lined by pseudostratified ciliated columnar epithelium
Pharyngobasilar fascia
Fill the gap between superior constrictor muscles and the base of the skull (Basiocciput)
Note:
Posteriorly it forms pharyngeal raphe (median raphe) which is attached to the pharyngeal tubercle (present on the inferior surface of the basilar part of occipital bone)
All the constrictor muscles of pharynx are inserted into
Pharyngeal raphe (median raphe)
Buccopharyngeal fascia
Covers the outer surface of the constrictor muscles of the pharynx
Between the muscular coat and the buccopharyngeal fascia, pharyngeal plexus of veins present.
Muscles of Pharynx
Outer circular layer made up of 3 constrictor muscles
- Superior pharyngeal constrictor muscle
- Middle pharyngeal constrictor muscle
- Inferior pharyngeal constrictor muscle
The three constrictors are so arranged that the inferior constrictor overlaps middle constrictor and middle constrictor overlaps the superior constrictor
Constrictor muscles origin arise from various sources
But all the constrictors muscle of pharynx are inserted into the median raphe (Pharyngeal raphe) on the posterior wall of the pharynx.
Tips:
The upper end of the median raphe is attached to the pharyngeal tubercle which is present in the inferior surface of the basilar part of the occipital bone
Inner longitudinal muscle layer
Consists of 3 muscles that run longitudinally
- Stylopharyngeus - arises from the styloid process
- Palatopharyngeus
- Salpingopharyngeus
Tips:
Tonsillar fossa is formed anteriorly by palatoglossus & posteriorly by palatopharyngeus
Muscles of soft palate
Palatoglossus
Palatopharyngeus
Function of constrictor muscles
All constrictor muscles contract reflexly during deglutition & induce a wave of peristalsis.
The cricopharyngeus acts as a sphincter & is normally kept closed except in deglutition.
Function of longitudinal layer
They elevate the larynx during swallowing, so that food is not passed to the larynx.
Palatopharyngeal muscle acts as a sphincter to close nasopharyngeal isthmus (junction between nasopharynx & oropharynx)
Structure in between pharyngeal muscle
Gap between the base of the skull, and superior constrictor muscle closed by pharyngobasilar fascia.
Structures passing through this gap:
- Auditory Tube
- Levator veli palatini muscle
Structure passing through gap of superior and middle constrictor muscles:
- Stylopharyngeus (by IX nerve)
- Glossopharyngeal nerve
The internal laryngeal nerve and the superior laryngeal vessels pierce the thyrohyoid membrane in the gap between middle and inferior constrictor muscles
The recurrent laryngeal nerve and the inferior laryngeal vessels pass through the gap between the inferior constrictor and the esophagus.
Blood supply of pharynx
Arterial Supply
- Ascending pharyngeal branch of external carotid artery
- Ascending and tonsillar branches of the facial artery
- Lingual branches of lingual artery
- Greater palatine, pharyngeal branches of the maxillary artery
Venous supply:
From pharyngeal venous plexus drain to internal jugular veins & facial veins
Notes
Facial, lingual & maxillary artery are branches of the external carotid artery.
Blood supply of palatine tonsil, soft palate & pharynx are somehow showing similarity.
Nerve supply of pharynx
Overall nerve supply of pharynx is derived from pharyngeal plexus
Motor supply
- By the cranial root of the accessory nerve through the vagus nerve except for stylopharyngeus which is supplied by the glossopharyngeal nerve.
- Parasympathetic secretomotor fibers from pterygopalatine ganglion.
Sensory supply
- General Sensory fibers mostly from glossopharyngeal nerve & partly by vagus
But nasopharynx supplied by branches from the pterygopalatine ganglion
- Taste sensation from vallecula and epiglottis area from the internal laryngeal, branch of the superior laryngeal nerve which is also the branch of the vagus.
Tips:
Pharyngeal plexus is formed by:
- Pharyngeal branch of vagus carrying fibers of the cranial root of the accessory nerve
- Pharyngeal branches of glossopharyngeal nerve
- Pharyngeal branches of superior cervical sympathetic ganglion
|
| Taste sensation from soft palate, pharynx and posteriormost part of the tongue is carried by the internal laryngeal, branch of the superior laryngeal nerve-branch of the vagus. |
| Nerve supply of pharynx and soft palate are quite relatable to each other. |
|
Pterygopalatine ganglion transmit parasympathetic secretomotor fibers to the lacrimal gland, glands of (soft palate, palate, pharynx, nasal cavity)
|
Development of Pharynx
Primitive gut
Extension: From the buccopharyngeal membrane cranially
To the cloacal membrane caudally.
It is divided into four parts
- Pharynx
- Foregut
- Midgut &
- Hindgut
The pharynx extended from buccopharyngeal membrane to the respiratory diverticulum(from where laryngotracheal tube develop to form larynx, Trachea, Lung)
Basic mechanism of Deglutition(Swallowing)
Food bolus is pushed through the oropharyngeal isthmus to oropharynx from the mouth cavity.
|
Nasopharyngeal isthmus is closed by elevation of the soft palate by levator veli palatini and tensor veli palatini.
This does not let the food bolus from entering the nose.
|
The inlet of the larynx is closed by epiglottis as the aryepiglottic fold is pulled backward by aryepiglottic and oblique aryepiglottic muscle.
|
Similarly, larynx and pharynx are elevated behind the hyoid bone by longitudinal muscles of pharynx and the food is pushed down over the posterior surface of the epiglottis, and close the inlet of larynx.
|
Food bolus is passed from pharynx to esophagus by contraction of constrictor muscles of pharynx inducing peristalsis movement.
Clinical Anatomy
|
Killian’s Dehiscence:
It is the potential gap between the oblique fibers of thyropharyngeus & the transverse fibers of the cricopharyngeus
Pharyngeal Diverticulum:
The mucosa of the pharynx may bulge & herniate through the potential space (Killian’s Dehiscence) due to muscular weakness resulting in pharyngeal diverticulum or pharyngeal pouch.
|
|
Tips:
Inferior constrictor muscles has two parts
- Thyro-pharyngeus part of inferior constrictor
- Crico-pharyngeus part of inferior constrictor
|
|
Retropharyngeal space:
It is the potential space between the posterior wall of the pharynx and prevertebral fascia, which separates the pharynx from the vertebral bodies.
Boundary/Relation
Anterior wall:
By the posterior wall of the pharynx
Posterior wall: By
Prevertebral fascia
Pre-vertebral muscle
Cervical vertebrae
Laterally:
Carotid sheath & Parapharyngeal space
Superiorly:
Basilar part of occipital bone
Inferiorly:
Continuous with Superior mediastinum
Content:
Retropharyngeal lymph node
Clinical importance:
- Bacterial infection from the mouth, nasopharynx, middle ear, teeth to this space leading to the formation of a retropharyngeal abscess (collection of pus within soft tissue)
- Blood, pus, air from this space can spread down into the superior mediastinum of the thorax.
|
| Difficulty in swallowing is known as dysphagia. |
| |
Comments (0)