MULTIPLE MYELOMA
Multiple myeloma is a malignant proliferation of plasma cells. Multiple myeloma is a chronic, progressive and fatal malignant condition in which the fundamental abnormality is a neoplastic proliferation of plasma cells that infiltrate the bone marrow and often other body tissues.
It comes under immunoproliferative disorder.
There are 3 major types of Proliferative disorders.
- Immunoproliferative disorder
- Myeloproliferative disorder
- Lymphoproliferative disorder
IMMUNOPROLIFERATIVE DISORDER:
Disorders characterized by abnormal proliferation of immunoglobulin-producing cells and abnormal proliferation of immunoglobulin monoclonal (M protein)represent part of the spectrum of disease due to the neoplastic behavior of the B lymphocyte series.
It is defined as a group of disorders arising from the abnormal proliferation of a single clone of immunoglobulin-secreting cells giving rise to paraproteinaemia.
Classification of Immunoproliferative Disorder:
A. Plasmacytic:
| Benign: Benign monoclonal gammopathy Essential cryoglobulinemia |
| Malignant: Multiple myeloma Solitary plasmacytoma Plasma cell leukemia |
| Nature unknown: Heavy chain disease Light chain disease |
B. Lymphocytic:
Benign:
- Essential hypergammaglobulinaemia
Malignant:
- Waldenstrom’s macroglobinaei
- Lymphoma
C. Others:
- Carcinoma of the lung, prostate,
- chronic lymphocytic leukemia
- Primary amyloidosis
Paraproteinaemia is a disorder characterized by abnormal proliferation of immunoglobulin-producing cells due to the neoplastic behavior of B-Lymphocytic series with an increase in serum level of homogenous immunoglobulin (monoclonal IG) or its fragments.
Paraprotein is the presence of a monoclonal immunoglobulin band (M-band) in the serum. It reflects the synthesis of immunoglobulin from a single clone of plasma cells.
Causes of paraproteinemia:
- Multiple myeloma
- Waldenstrom’s macroglobulinemia
- Heavy chain disease
- Benign monoclonal gammopathy
- Primary amyloidosis
- Non-Hodgkin’s lymphoma
- Chronic lymphocytic leukemia
Multiple myeloma
Multiple myeloma is a chronic, progressive and fatal malignant condition in which the fundamental abnormality is a neoplastic proliferation of plasma cells that infiltrate the bone marrow and often other body tissues.
It is a malignant proliferation of plasma cells.
|
Plasma cells are derived from B lymphocytes and produce immunoglobulin (Ig) which contains heavy and light chains. Normally Ig molecule consists of 4 polypeptide chains 2 heavy chains and 2 light chains.
Each Ig molecules have either 2 kappa or 2 lambda light chains. In myeloma, plasma cells produce monoclonal (M) Ig of a single heavy and light chain commonly referred to as a paraprotein. The most common abnormality is the production of excess of light chains over heavy chains. The excess light chains are secreted into the extracellular fluid and readily pass through the glomerulus. Light chains are catabolized by renal tubular cells but when present in excess pass into the urine as Bence Jones Protein. The most common monoclonal Ig (M protein) is:
|
Clinical features of Multiple Myeloma
Clinical features of Multiple Myeloma developed due to tissue infiltration, production of a large number of paraprotein, and impairment of immunity.
Myeloma is a disease of middle and old age (50-70 years), male predominance.
1. Bone:
- Bone pain and tenderness
- Skeletal deformity
- Osteoporosis
- Pathological fracture
(Bone becomes soft due to infiltration and proliferation of myeloma cells causing destruction of medullary and cortical bone and causing osteolysis due to increased osteoclastic activity by a factor released by myeloma cells).
2. Anemia: Due to the dilutional effect of a large amount of paraprotein in circulation, depression of erythropoiesis by infiltration of myeloma cells in the bone marrow, and the effects of cytotoxic drugs.
3. Infection: Due to subnormal levels of normal Ig and suppression of the normal antibody
4. Bleeding manifestation: Due to platelets suppression and paraprotein causes abnormal platelets function
5. Renal insufficiency: Due to the deposition of antibody-derived materials in the kidney
6. Nervous system manifestations like quadriplegia, and paraplegia due to compression by collapsed vertebrae or myeloma tissue.
Laboratory diagnosis of Multiple Myeloma
1. Routine blood examination:
- Hb: Usually decreased
- ESR: High (due to paraprotein that causes increased rouleaux formation).
- TC of WBC: Normal / Increased / Decreased
- RBC: Decreased
- Platelets: Decreased
2. Peripheral blood film: (Shows leucoerythroblastic blood picture with an abnormally blue-stained background in the blood film).
- RBC: Normochromic normocytic red cells with the marked rouleaux formation with few nucleated cells present
- WBC: Immature granulocytic cells and a small number of myeloma cells may present
- Platelets: Reduced
3. Bone marrow examination:
- Cellularity: Hypercellular
- M:E: Increased
- Erythropoiesis: Depressed but normoblatic
- Granulopoiesis: Presence of myeloma cells both mature and immature (15-30% or more).
- Megakaryopoiesis: Decreased
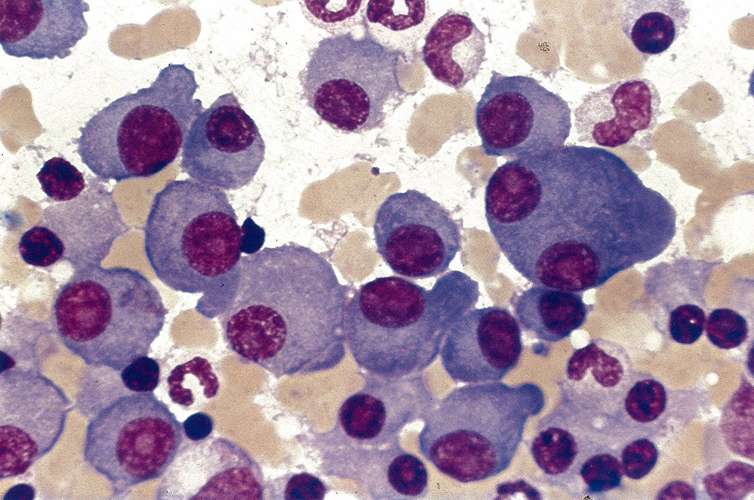
Fig: Clusters of plasma cells in multiple myeloma in bone marrow smear
4. Biochemical findings:
- Serum total protein: Markedly increased
- Serum albumin: Reduced
- Serum globulin: Increased
5. Electrophoresis:
- Serum protein electrophoresis: The paraprotein appear as a single narrow homogenous M band
- Immunoelectrophoresis: (types of light and heavy chains can be identified by using this test). IgG 50%, IgA 25%, and IgD 1% are present in most cases.
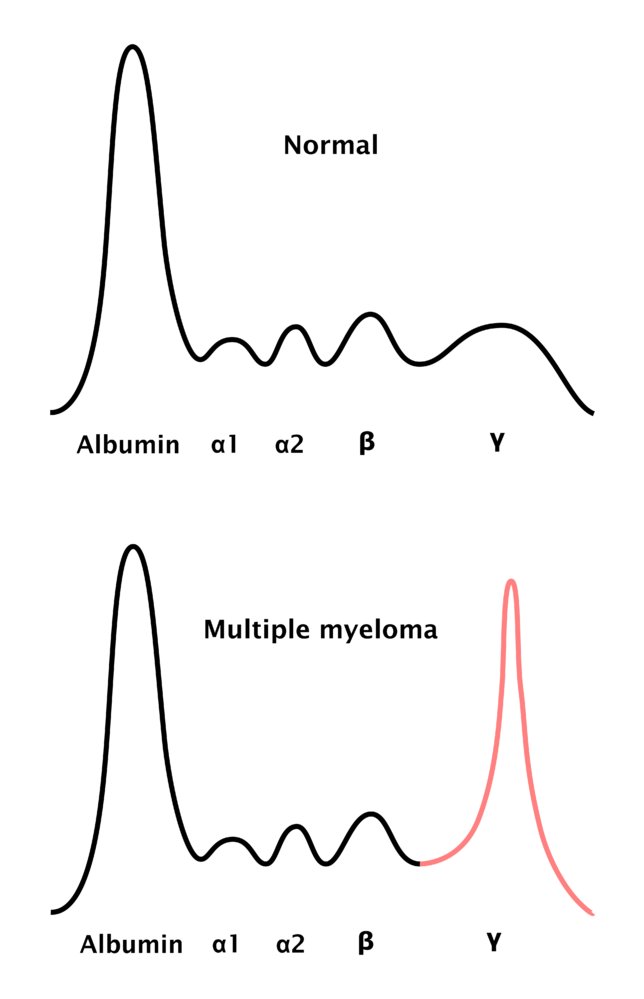
Fig: Electrophoresis in multiple myeloma - the monoclonal antibodies cause a peak in the gamma-globulin zone of the electrophoresis, which is termed M protein (also M component, myeloma protein, spike protein, and paraprotein).
6. Urine examination:
Detection of Bence Jones Protein in urine.
7. Radiological findings:
Osteolytic lesions appear as multiple rounded discrete punched-out areas with no sclerosis at the margin. They occur most frequently in bones normally containing red marrow, particularly in the skull and pelvic bones.
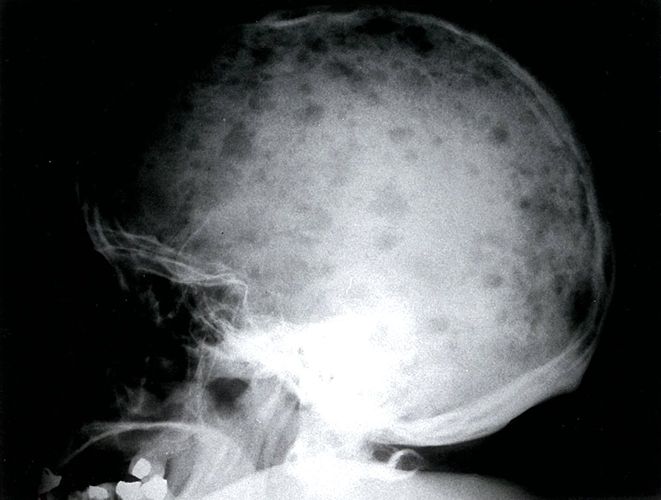
Fig: Multiple punched-out lytic lesions in X-ray skull of a patient with a history of multiple myeloma
Diagnostic criteria of multiple myeloma:
1. Osteolytic lesion in bone (Seen on X-ray)
2. Detection of monoclonal protein (M protein or paraprotein in serum or urine).
3. Increased proliferation of plasma cells with immature form in bone marrow
- Myeloma cells: Myeloma cells vary in appearance from small mature differentiated cells resembling typical plasma cells to large, immature undifferentiated cells of 20-30 micrometers in diameter.
- Mature cell: Mature cells in bone marrow have basophilic cytoplasm sometimes with perinuclear halo, eccentric nucleus, and chromatic is arranged in coarse stands although seldom show cartwheel appearance.
- Immature cells: The cytoplasm of immature cells is abundant, light blue, and may show a perinuclear halo, vacuolation, and Russell bodies with finer evenly distributed chromatin. Nucleoli are common.
Causes of increased plasma cells in bone marrow:
- Multiple myeloma
- Aplastic anemia
- Rheumatoid arthritis
- Liver cirrhosis
- Sarcoidosis
- Secondary carcinoma
- SLE
- Chronic inflammation
Bence Jones Protein:
It is an immunoglobulin light chain either kappa or lambda, excreted in urine and found in various pathological conditions.
Free monoclonal kappa or lambda light chain of immunoglobulin appears in the urine as Bence Jones Protein.
Properties of Bence Jones Protein:
- It coagulates at a temperature between 50-60ºc.
- It disappears at 100ºc while all other protein
- It again appears at 50-60ºc on cooling.
Detection of Bence Jones Protein:
- Heat precipitation test
- Electrophoresis
Bence Jones Protein Found in:
|
Heat precipitation test/ Fluctuation test:
- 5ml of urine is taken to a test tube and placed in a water bath.
- The temperature increased gradually when the temperature reached at 40ºc -60ºc precipitation/ coagulate begins to appear then the temperature rises up to the boiling point (100ºc) and the precipitation will disappear.
- If the precipitate/coagulates disappear then it is sure that the protein is BJP because normal serum protein coagulates at a temperature over 60ºc where BJP disappears.
- Precipitation will reappear during the cooling of the specimen.
Read also
A vape clutch is a type of vape mod that is designed to be sleek and compact, making it easy to carry around in a pocket or purse. It typically features a single battery and a simple button mechanism to activate the device. The small size of a vape clutch makes it an ideal choice for vapers who are always on the go and need a device that is easy to transport. However, the compact size of a vape clutch can also limit the battery life and overall power of the device compared to larger mods. Vape clutches come in a variety of designs and colors, making it easy for vapers to find one that suits their personal style

Comments (0)