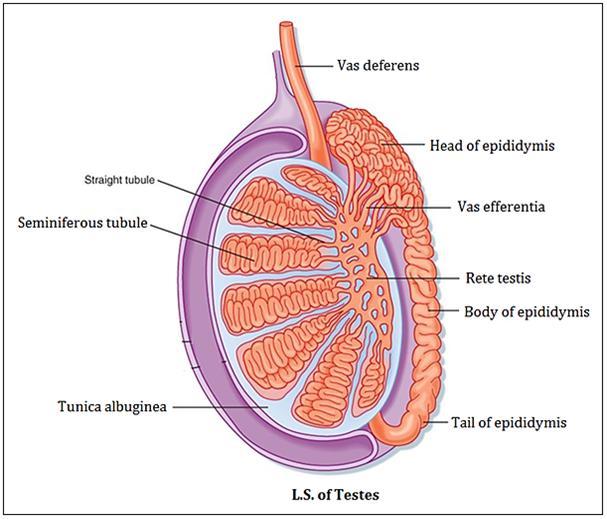
Testis
Male genital system
| External genital organ - Penis - Scrotum |
| Internal genital organ - Testis - Epididymis - Prostrate - Bulbourethral glands - Seminal vesicle - Ejaculatory duct - Urethra - Vas deferens |
Testis
It is a male gonad. It is homologous with the ovary in the female.
Functions of the testis:
| Production of spermatozoa |
| Secretion of testosterone (male hormone) |
| Responsible for the development and maintenance of the secondary sex characteristics of male. |
External features:
Two surfaces - Medial and Lateral
Two poles - Upper and Lower. The upper pole provides attachment to the spermatic cord.
Two borders - Anterior and Posterior
The anterior border is covered by the tunica vaginalis. The posterior border is covered partly by the tunica vaginalis. It provides attachment to the epididymis. Laterally, the epididymis is separated from the testis by the extension of the cavity of tunica vaginalis called the 'sinus of the epididymis.
Coverings of Testis
There are 3 coverings of the testis. From superficial to deep:
| Tunica vaginalis It is a serous sac that represents the lower persistent portion of the processus vaginalis. It covers the whole testis except its posterior border. |
| Tunica albuginea It is a thick, dense layer of fibrous tissue enclosing the testis. It is covered by the visceral layer of tunica vaginalis except where it is in direct contact with the epididymis. |
| Tunica vasculosa It is the innermost vascular layer of the testis, lining the lobules of the testis. |
Structure of Testis:
The testis is enclosed in a fibrous capsule, the tunica albuginea. The posterior border of the tunica albuginea forms an incomplete vertical septum, called 'mediastinum testis'. Numerous septa extend from the mediastinum to the inner aspect of the tunica albuginea and incompletely divide the testis into 200-300 lobules. Each lobule contains 2 - 4 coiled seminiferous tubules. Seminiferous tubules join each other and form straight tubules.
Cells in the testis:
| Spermatogenic cells - produce spermatozoa |
| Sertoli cells - give support & nutrition to the developing spermatogenic cells |
| Interstitial cells of Leydig - secrete testosterone |
Arterial supply of testis
| Mostly supplied by the testicular artery, branch of the abdominal aorta. |
| Partly supplied by the artery of vas deferens, a branch of the superior or inferior vesical artery. |
| Sometimes, supplied by the cremasteric artery, a branch of the inferior epigastric artery. |
Venous drainage of testis
Some veins appear from the posterior border of the testis and epididymis, and unite to form a "PAMPINIFORM PLEXUS"
At the superficial inguinal ring, the plexus unites to form 4 veins, which pass through the inguinal canal within the spermatic cord, and at the deep inguinal ring they further join to form 2 testicular veins, which accompany the testicular artery.
Right testicular vein drains into the inferior vena cava at an oblique angle and the left testicular vein drains into the left renal vein at a right angle.
Lymphatic drainage of testis
The lymph vessels from the testis ascend along the testicular vessels in the spermatic cord and drain into pre-aortic and para-aortic lymph nodes.
Clinical correlation
Hydrocele: It is the accumulation of the fluid within the tunica vaginalis.The fluid may cause inflammation of the testis.
Varicocele: It is a clinical condition in which veins of the pampiniform plexus become dilated, tortuous and elongated. It commonly affects adolescents and young adults.
Development of testis
The testis develops in the abdominal cavity on its posterior wall from the mesodermal "GENITAL RIDGE".
All the components of the testis {tunica albuginea, fibrous septa, seminiferous tubules, straight tubules, rete testis, and Sertoli cells} develop from the genital ridge except primordial germ cells (spermatogonia) which develop from the wall of the yolk sac.
Descent of testis
The testis develops in the lumbar region on the posterior abdominal wall. Later they descend through the pelvis and inguinal canal during the 7th and 8th months of fetal life.
Time of descent:
| Descent of testis begins in the 2nd month of intra-uterine life. |
| Reaches the iliac fossa by the 4th month. |
| At the 7th month, it reaches the deep inguinal ring. |
| Transverses the inguinal canal during the 8th month. |
| Finally, reaches the scrotum at or slightly after birth. |
Factors responsible for descent of the Testis
| Contraction of the gubernaculum (a band of loose fibromuscular tissue extending from the lower pole of the testis to the base of the scrotum). |
| Increase intra-abdominal pressure and temperature. |
| Hormones (eg.Testosterone) |
| Differential growth of the body wall |
Also read: Anatomy Question Collection
Also read: Anatomy Questions & Answers
Also read: Anatomy notes

Comments (0)