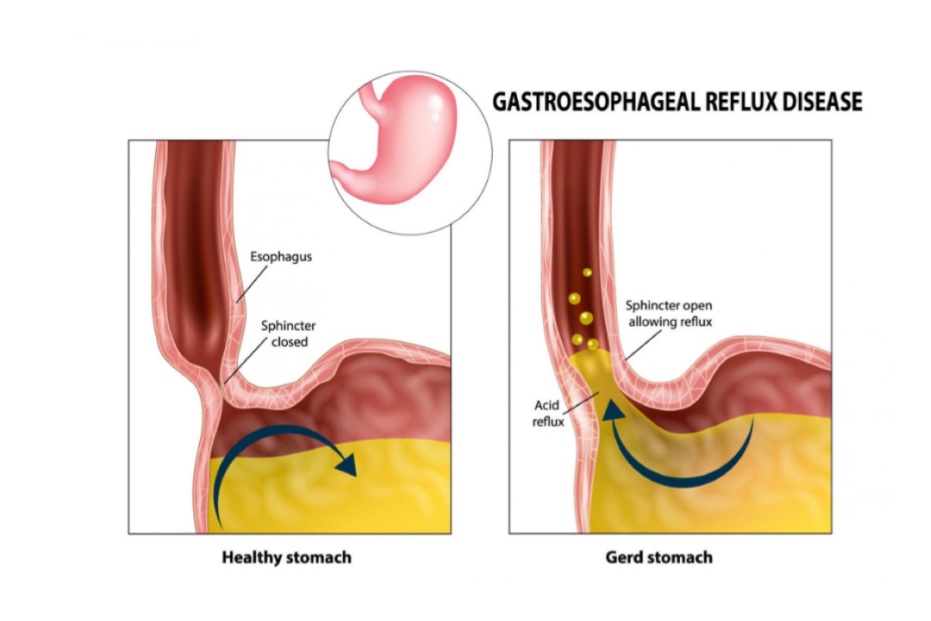
OESOPHAGUS
Q.1 What is the length of the oesophagus?
25 cm
Q.2 What is the extent of oesophagus?
- It begins in the neck at the level of the lower border of C5 vertebra, i.e. at the lower border of the cricoid cartilage.
- It ends in the abdomen at the level of the lower border of the T11 vertebra, at the cardiac orifice of the stomach.
Q.3 What are the ‘Curvatures of oesophagus’?
Esophagus shows.
- Two side to side curvatures towards left.
– At root of neck.
– Oesophageal opening in diaphragm.
- Anteroposterior curvature:
Follows the curvature of the spine.
Q.4 What are the sites of oesophageal constrictions?
- At its commencement:
6 inches from incisor teeth. - Where it is crossed by aortic arch:
9 inches from incisor teeth. - Where it is crossed by left bronchus:
11 inches from incisor teeth. - At its termination:
15 inches from incisor teeth.
Q.5 Name the structures intervening between the oesophagus and vertebral column.
- Thoracic duct
- Vena azygos
- Hemiazygos vein
- Accessory hemiazygos vein
- Right posterior intercostal arteries
Q.6 What are the divisions of oesophagus?
The esophagus is divided into three parts:
- Cervical,
- Thoracic and
- Abdominal
Q.7 What is the relation of recurrent laryngeal nerves to the oesophagus in the neck?
The right and left recurrent laryngeal nerves lie anterolateral to the esophagus in corresponding grooves between it and the trachea.
Q.8 What is the blood supply of oesophagus?
Arterial supply:
- Cervical part: Inferior thyroid artery.
- Thoracic part: Oesophageal branches of aorta and bronchial arteries.
- Abdominal part: Oesophageal branches of the left gastric artery.
Venous drainage:
- Cervical part: Into brachiocephalic vein.
- Thoracic part: Into the azygous vein.
- Abdominal part: Into portal vein through the left gastric vein. The lower end is the site of porto-systemic anastomosis.
Q.9 What is the nerve supply of oesophagus?
Parasympathetic nerves:
Sensorimotor and secretomotor.
Upper ½: Recurrent laryngeal nerve.
Lower ½: Oesophageal plexus formed by two vagus nerves.
Sympathetic nerves:
Vasomotor
Upper ½: Fibres from middle cervical ganglion.
Lower ½: Fibres from upper 4 thoracic ganglia.
Q.10 What is ‘Achalasia cardia’?
It is a condition of neuromuscular incoordination in which the lower end of the oesophagus fails to dilate when food is swallowed. As a result, food accumulates in the esophagus.
Q.11 What is the clinical importance of constrictions of the oesophagus?
- During endoscopy, these constrictions should be kept in mind.
- These are also the sites of development of strictures usually.
Q.12 What are oesophageal varices and what is their clinical importance?
These are the dilatations of the oesophageal veins in portal hypertension, which form an anastomosis between azygos (systemic) and left gastric (portal) veins.
Clinical importance:
These may rupture leading to severe hemorrhage.
Q.13 What is the effect of enlargement of the left atrium on oesophagus?
In mitral stenosis, enlargement of the left atrium causes backward displacement of the esophagus, which can be seen in a barium swallow.
Q.14 How oesophagus is developed?
The esophagus is developed from the part of foregut lying between pharynx and stomach.
It is at first short but later on elongates with the descent of diaphragm and formation of neck.
Q.15 What are the characteristic histological features of oesophagus?
From within outwards, it is made up of:
- Mucosa: Lined by stratified squamous epithelium.
- Submucosa: Contains mucous glands.
- Muscular layer: Has external longitudinal and inner circular fibers.
The muscle fibers are striated in the upper two thirds and smooth in the lower one third.
- Connective tissue sheath of areolar tissue.
Also read: Anatomy Question Collection
Also read: Anatomy Questions & Answers
Also read: Anatomy notes

Comments (0)