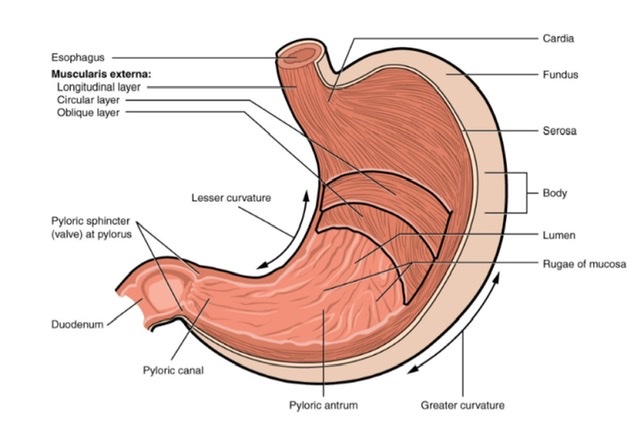
Stomach (Viva)
STOMACH
Q.1 What is the position of the stomach?
It lies obliquely in the upper and left part of the abdomen, occupying epigastric, umbilical, left hypochondrium, and left lumbar region.
Q.2 What are the normal variations in the capacity and shape of the stomach?
Capacity: At birth: 30 ml
At puberty: 1000 ml
In adults: 1.5-2 liters
Shape:
When empty: J-shaped
When distended: Pyriform
In obese: More horizontal (Steerhorn stomach)
Q.3 What are the different parts of the stomach?
- Cardiac part: Subdivided into:
– Fundus: Part of the stomach lying above the cardio esophageal junction.
– Body
– Pyloric part: Subdivided into:
Pyloric antrum
Pyloric canal
Stomach has:
two orifices: Cardiac and pyloric
two curvatures: Lesser and greater
two surfaces: Anterior and posterior
Q.4 How the pyloric orifice is recognized by a surgeon?
By:
- Circular groove (Pyloric constriction) produced by pyloric sphincter which feels like a firm ring
- Prepyloric vein: Lies anteriorly in pyloric constriction
Q.5 What is the level of orifices of the stomach?
Cardiac orifice (Physiological sphincter): T11 vertebra.
Pyloric orifice: L1 vertebra.
Q.6 Name the ‘bare areas’ of stomach?
- Greater and lesser curvatures, along the peritoneal reflections.
- Triangular area on the posterior surface close to the cardiac orifice and related to the left crus of the diaphragm.
Q.7 Name the structures forming the ‘Stomach bed.’.
These structures are related to the posterior surface of the stomach.
- Spleen: Related to the fundus and is separated by the cavity of the greater sac.
- Other structures are separated by the cavity of lesser sac:
– Diaphragm
– Left suprarenal
– Left kidney
– Splenic artery
– Pancreas
– Transverse mesoscolon
– Splenic flexure of colon
Q.8 What is the blood supply of the stomach?
Arterial supply :
- Left gastric artery: Branch of coeliac trunk
- Right gastric artery: Branch of gastroduodenal artery
- Right gastroepiploic artery: Branch of common hepatic
- Left gastroepiploic artery: Branch of splenic.
- Short gastric arteries: Branches of splenic.
Venous drainage:
Into superior mesenteric and splenic veins, which pass into the portal vein.
Q.9 What is the lymphatic drainage of the stomach?
For lymphatic drainage, the stomach is divided into four regions by imaginary lines as follows:
- Draw a vertical line just to the left of the cardio esophageal junction. It drains into pancreaticosplenic nodes, which drain into coeliac nodes.
- Draw a vertical line separating the pyloric part from the body. The area between two vertical lines is divided into upper 2/3 and lower 1/3 by a curved line parallel to greater curvature.
Upper 2/3 is drained by left gastric nodes, which drain into coeliac nodes and lower 1/3 drains into right gastroepiploic nodes which in turn drain into pyloric nodes, then hepatic nodes and finally coeliac nodes. - The pyloric part drains into pyloric, hepatic, and left gastric nodes which in turn drain into coeliac nodes.
From coeliac nodes, it passes to intestinal lymph trunk to reach cisterna chyli.
Q.10 What is the nerve supply of the stomach?
- Sympathetic nerves: T6–T10 segments from coeliac plexus.
These are:
– Vasomotor,
– Motor to pyloric sphincter,
– Chief pathway for pain sensation.
- Parasympathetic nerves: Vagus as:
– Anterior gastric nerve (mainly left vagal fibers):
Supplies anterior surface of fundus and body of the stomach, pylorus, and pyloric antrum.
– Posterior gastric nerve (mainly right vagal fibers):
Supplies posterior surface of fundus, body, and pyloric antrum and gives a branch to coeliac plexus.
These are motor and secretomotor to stomach.
Q.11 What are ‘nerve of Latarjet’?
Anterior and posterior vagi are also known as nerves of Latarjet.
Q.12 What are the functions of the stomach?
- As a reservoir of food
- Digestion: Mainly breakdown of proteins to peptones
- As antiseptic acid barrier: By HCl
- Self-protection: From HCl by mucus
- Absorption: Salt, water, alcohol and certain drugs
- Secretion of intrinsic factor of Castle.
Q.13 What is the advantage of highly selective vagotomy?
It does not cause stomach atony. Branches that supply the acid-secreting body of the stomach are only cut, thus preserving innervation and function of pyloric antrum.
Q.14 In which part of the stomach, X-ray shows gas?
Fundus of stomach which appears as a dark shadow below the left dome of the diaphragm.
Q.15 What is gastric canal? What is its clinical importance?
These are the mucosal folds (Rugae) along the lesser curvature which are arranged longitudinally to form a canal. Clinical importance: Gastric canal allow rapid passage of fluid along the lesser curvature to the lower part before it spreads to other parts of the stomach. Thus it is irritated most by the swallowed liquids and hence it is more vulnerable to peptic ulcers.
Q.16 What are the different types of glands in the stomach?
- Cardiac glands: Tubular glands.
- Glands of body and fundus: Tubular glands.
- Pyloric glands: Convoluted tubular glands.
Q.17 What are the cell types present in glands of the stomach?
- Mucous cells:
Secrete mucous. Present in pyloric antrum and pyloric canal. - Zymogen cell (Chief cells):
Present in glands of fundus and body. Secrete gastric enzymes. - Oxyntic cells (Parietal cells):
Present in glands of fundus and body; secrete HCl - Mucous neck cells:
Present at neck of glands; Secrete mucus - Argentaffin cells:
Present at base of gastric glands of the fundus. Secrete gastrin and serotonin.
Q.18 What is ‘leather bottle stomach’?
Thickening of stomach wall due to the proliferation of fibrous tissue especially in the submucosa. The mucous membrane appears normal.
Q.19 What is the commonest site of gastric ulcers?
Gastric ulcers are usually found in the distal part, near the lesser curvature.
Q.20 What is the cause of fatal haemorrhage in perforated gastric ulcer?
Perforation of a gastric ulcer on the posterior wall of the stomach can lead to erosion of splenic artery leading to fatal hemorrhage.

Comments (0)