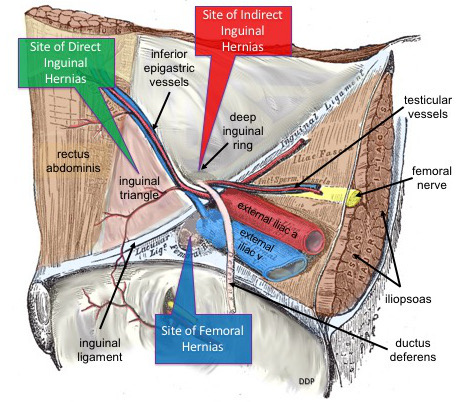
Femoral Triangle (Viva)
FEMORAL TRIANGLE
Q.1 Why femoral triangle is known as Scarpa’s triangle?
Because it was first described by Antonio Scarpa (1747-1832) in Italy.
Q.2 What are the boundaries of the femoral triangle?
It is bounded by
- Laterally: Medial border of sartorius.
- Medially: Medial border of adductor longus.
- Base: Inguinal ligament.
- Apex: Directed downwards and is formed by the meeting of medial and lateral boundaries.
- Roof:
– Skin,
– Superficial fascia and
– Deep fascia. - Floor:
– Laterally by iliacus and psoas major.
– Medially by adductor longus and pectineus.
Q.3 What are the contents of the femoral triangle?
- Femoral artery
- Branches of femoral artery:
– Deep branches: Profunda femoris, deep external pudendal, descending genicular, saphenous, and muscular.
– Superficial branches: Superficial external pudendal, superficial epigastric and superficial circumflex iliac.
- Femoral vein (medial to the artery) and its tributaries
- Femoral sheath
- Femoral nerve (lateral to the artery)
- Nerve to pectineus
- Femoral branch of genitofemoral nerve
- Lateral cutaneous nerve of thigh and
- Deep inguinal lymph nodes.
Q.4 What is femoral sheath?
It is a funnel-shaped fascial sleeve enclosing the upper 1½ inches of the femoral vessels.
Q.5 How is femoral sheath formed?
It is formed by the downward extension of the abdominal fasciae. The anterior wall is formed by fascia transversalis and posterior wall by fascia iliaca.
Q.6 What are the relations of the femoral sheath?
Anterior:
- Skin
- Superficial fascia and
- Deep fascia with saphenous opening and great saphenous vein.
Posterior:
- Iliopectineal fascia
- Pectineus and
- Iliopsoas.
Lateral:
- Femoral nerve and
- Iliacus.
Medial:
- Lacunar ligament
- Pectineus and
- Pubic bones.
Q.7 What are the parts of the femoral sheath?
The cavity within the femoral sheath is divisible in three parts.
Lateral part contains the femoral artery and a femoral branch of the genitofemoral nerve.
Middle part contains the femoral vein and the medial part is called the femoral canal.
Q.8 What is the femoral canal?
It is the medial compartment of the femoral sheath. It is conical and ½ inch wide at the base and ½ inch long.
Q.9 What is the femoral ring?
The base or upper end of the femoral canal is called the femoral ring. The femoral ring is filled by condensed extraperitoneal tissue, the femoral septum, containing a lymph node and covered by parietal peritoneum.
Q.10 What are the boundaries of the femoral ring?
- Anterior: Inguinal ligament.
- Posterior: Pectineus and its fascia.
- Lateral: Septum separating it from the femoral vein.
- Medial: Concave margin of lacunar ligament.
Q.11 What are the contents of the femoral canal?
- Lymph node (of Cloquet or of Rosenmuller).
- Lymphatics.
- Areolar tissue.
Q.12 What are the functions of the femoral canal?
- It serves as a dead space for the expansion of the femoral vein.
- It allows a lymphatic pathway from the lower limb to the external iliac lymph nodes.
Q.13 What structure is drained by the lymph node of the femoral canal?
Glans penis in the male and clitoris in females.
Q.14 What is the clinical importance of the femoral canal?
The femoral canal is a potential point of weakness in the lower abdominal wall through which a viscus (intestines or urinary bladder) may protrude and give rise to a femoral hernia.
Q.15 Why is a femoral hernia commoner in females?
Because the femoral canal is larger in the females due to the greater width of the pelvis and smaller size of the femoral vessels. In the females, there is a rise in intraabdominal pressure due to pregnancy predisposing to femoral hernia.
Q.16 Why is strangulation more common in femoral hernia?
Because the neck of the femoral canal is narrow.
Q.17 What is the risk of enlarging the opening of the femoral canal in releasing the strangulation of a femoral hernia?
In order to enlarge the opening of the femoral canal the sharp lateral edge of the lacunar (Gimbernat’s) ligament may require an incision. An abnormal obturator artery may occasionally be present, which passes behind the lacunar ligament and is then in danger of being cut.
Q.18 What are the coverings of femoral hernia?
From within outwards:
- Peritoneum
- Femoral septum
- Femoral sheath
- Cribriform fascia
- Superficial fascia
- Skin
Also read: Anatomy Question Collection
Also read: Anatomy Questions & Answers
Also read: Anatomy notes

Comments (0)