Muscular Tissue
5 years ago 5460
|
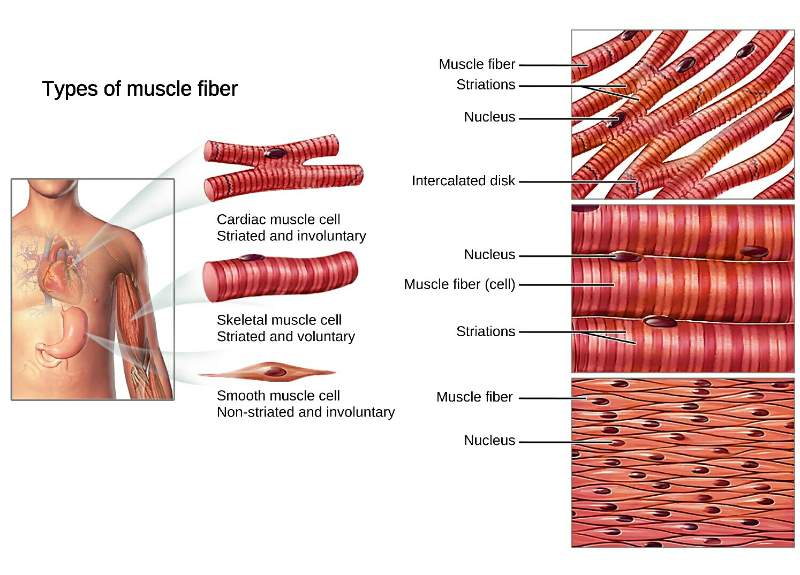
• Smooth/visceral muscle
(Involuntary, non-striated)
|
|
• Skeletal/somatic muscle
(Voluntary, striated)
|
|
• Cardiac, heart muscle
(Striated)
|
Histological Classification of Muscle
| • Striated Muscle Eg. Skeletal muscle, Cardiac muscle |
| • Non-striated Muscle Eg. Smooth muscle |
| Skeletal muscle (Body wall muscle) |
Cardiac muscle (Heart muscle) |
Smooth muscle (Visceral muscle) |
| Voluntary, striated muscle | Involuntary, striated muscle | Involuntary, non-striated muscle |
| Long cylindrical, Unbranched | Short cylindrical, branched | Spindle-shaped, unbranched |
| Multiple peripheral nucleus | Single central nucleus | Single central nucleus |
| Cross striation present | Cross striation present | No cross striation |
| Develop from somatic mesoderm | Develop from splanchnic mesoderm | Develop from mesenchyme |
| Intercalated disc absent | Intercalated disc present | Intercalated disc absent |
| Found in locomotor muscles, muscles of abdominal wall, diaphragm | Found in heart muscle (form myocardium) | Found in the alimentary, respiratory, urinary tract, blood vessels, ciliary muscle |
|
Epicardium
Formed by the visceral layer of the serous pericardium
of (Simple Squamous Epithelium)
|
| Middle Myocardium Muscular layer of cardiac Muscle |
|
Endocardium (innermost layer of the heart) is
of (Simple Squamous Epithelium)
|
|
• Multiple nuclei are found at the periphery of the muscle fiber of skeletal muscle under sarcolemma.
• The number & location of nuclei present in skeletal helps to discriminate skeletal muscle from cardiac & smooth muscle.
|
|
Epimysium:
Connective tissue cover around the entire muscle
|
|
Perimysium:
Connective tissue covering around each fascicle (bundle of muscle fibers)
|
|
Endomysium:
Connective tissue sheaths surrounding each muscle fiber
• Below the endomysium, there is sarcolemma (plasma membrane of muscle fibers) Each muscle fibers is surrounded by outer endomysium and inner sarcolemma. |
| • Epimysium cover (Whole skeletal muscle - composed of muscle fascicles) |
| • Perimysium cover (Muscle fascicle - contains a bundle of muscle fibers) |
| • Endomysium & sarcolemma cover (Muscle fibers - composed of myofibrils) Myofibrils are present within the cytoplasm of muscle fibers called sarcoplasm. |
|
• Each muscle is composed of a bundle of muscle fibers called muscle fascicle.
• Muscles fascicle:
Bundle of muscles fibers
|
| • Each muscle fibers is surrounded by outer endomysium and inner sarcolemma. |
| • Cytoplasm of muscle fibers known as sarcoplasm. |
| • The sarcoplasm (cytoplasm) is filled with numerous longitudinal fibrils, called myofibrils. |
| • Each myofibril is composed of 2 types of myofilaments. |
|
• Thin actin filament (composed of a protein called actin)
• Thick myosin filament (composed of a protein called myosin)
|
| ♦Due to the alternation presence of thin actin & thick myosin filament, skeletal muscle has striated appearance (alternation dark & white bands). |
| During contraction of muscle, heads of Thick myosin filament (which lie in the middle area of sarcomere) pull the thin actin filaments from both (either side) towards itself, shortening the length between two successive Z-lines, thus called sarcomere as a functional contractile unit of muscle fibers. |
|
• I bands: Thin actin filament only
|
| • Z line: Bisect the I band |
| • A bands: overlapping area of thick (myosin) & thin (actin) filament |
| • M line: Bisect the A band |
| • Sarcolemma (cell membrane) - surrounded by endomysium • Multiple peripheral nucleus are present beneath the sarcolemma • T tubules - (vertical invagination of sarcolemma separating A Band & I band) |
| • T tubules - carries motor stimulus from sarcolemma into the myofibrils |
| • Sarcoplasm (Cytoplasm of muscle fiber) |
| • Sarcoplasmic reticulum - a type of smooth endoplasmic reticulum • Store Ca++ ions and releases to sarcoplasm through terminal cisterns on receiving motor stimulus through T tubule • Terminal cisterns (enlarged area of sarcoplasmic reticulum around the transverse T tubules) |
| • Triad (2 terminal cisternae + T tubule) |
| • Terminal cistern - releases available Ca+ into the sarcoplasm (cytoplasm) |
|
• Mitochondria - produce ATP requiring glucose & O
• Also known as sarcosome
|
| • Glycosome
Granules of stored of glycogen
|
|
•Myoglobin
- red-pigmented protein, store oxygen within muscle |
| • Myofibrils
Each myofibril is composed of longitudinal protein filaments called myofilaments.
|
| Actin - present in thin actin filament |
| Myosin - present in thick myosin filament |
| Muscle Protein found in Dark & Light band • Dark Band: Myosin • Light Band: Actin, Troponin, Tropomyosin |
| Tropomyosin covers myosin binding sites of actin filaments. |
| Troponin needs to bind with Ca+ to pull the Tropomyosin off of the binding site. |
| • Troponin T protein - bind with tropomyosin to form tropomyosin complex • Troponin C protein - bind with Ca++ |
| Skeletal muscle is composed of bundles of very long, cylindrical, multi-nucleated cells, called muscle fibers. |
| Skeletal muscle is voluntary, because the stimulation for their contraction & relaxation is under conscious control. |
| The cell membrane of muscle fiber is known as sarcolemma. |
| The cytoplasm of muscle fiber is called sarcoplasm. |
| In sarcoplasm there is an extensive smooth endoplasmic reticulum called sarcoplasmic reticulum. |
| The sarcoplasm is filled with numerous longitudinal fibrils called myofibrils. |
| Each myofibril has A band (darker band) & I band (lighter band). |
| Each myofibril is composed of longitudinal protein filaments called myofilaments. |
| Multiple nuclei are found at the periphery of muscle fiber under sarcolemma. |
| In cell | In muscle |
| Plasma membrane | Sarcolemma |
| Endoplasmic reticulum | Sarcoplasmic reticulum |
| Cytoplasm | Sarcoplasm |
| Mitochondria | Sarcosome |
| Means muscle is in quite in tension even in resting state. |
| Therefore, a muscle is not completely relaxed even in the resting condition. |
| Motor nerve supply of voluntary muscle |
| Alpha motor neuron - supply extra-fused fibers of muscle that produce movement. |
| Gamma motor neuron - supply intrafusal fibers of muscle spindle for the maintenance of muscle tone. |
| Functional Contractile Unit of Muscle - Motor Unit |
| Functional Contractile Unit of Muscle Fiber - Sarcomere |
|
• Short & cylindrical branching
• Striated involuntary muscle
• Single oval nucleus lie centrally
|
| • Each fiber in a network is separated from the next fiber by an irregular transverse intercalated disc. |
| • Found in myocardium & in the walls of the large vessels joining the hearts |
| This means a single cell containing multiple nuclei; all nuclei sharing the same cytoplasm bounded in the same cell membrane. |
| Commonly, syncytium is formed merging of several cells together losing their individual cell membrane; bounded in a single large cell membrane but retaining their nuclei. |
| • Due to the lack of multiple separate cell membranes, make the quick transmission of impulses between nuclei. |
| • Faster the impulse transmit, faster will be the contraction of muscle |
| The formation of skeletal muscle is an example of true syncytium. |
| A single large muscle fiber is formed by the fusion of several thousand muscle cells. |
| That’s why skeletal muscle fibers have multiple peripheral nuclei. |
| Cardiac muscle does not form true syncytium because each muscle fiber is composed of end to end connection of the individual muscle cells. |
| These cells are not merged into single giant cell & separate by their own cell membrane. |
| Presence of multiple cell membranes act as barriers for impulses to transmit faster from one cell to another. But still whole cardiac muscle contract as a single unit. |
| Because cardiac muscle act as functional syncytium due to the presence of intercalated disc connecting each fiber. |
| Intercalated disc contains abundant gap junctions (a type of channel), which form electrical synapses, allowing contraction signals to pass from cell to cell as a single wave and as a whole cardiac muscle contract as a single unit. |
| Single skeletal muscle fiber is the example of true syncytium and follow All-or-None law. |
| But whole cardiac muscle is the example of functional syncytium and follow All-or-None law. |
| Each fiber in a network of cardiac muscle is separated from the next fiber by an irregular transverse thickening of the sarcolemma is called intercalated disc. At sites of end-to-end contact are called intercalated discs. |
| Only found in cardiac muscle; special characteristic feature of cardiac muscle. |
| • It has abundant desmosomes & other adherent junctions which hold one cell to adjacent cells firmly together. |
| • It also contains abundant gap junctions, which form electrical synapses allowing contraction signals to pass from cell to cell as a single wave. |
| • Connect actin filaments in myofibrils of one cell to next. |
| Why cardiac muscles never get fatigued, but the skeletal muscle get fatigued? |
| Because there is plenty of mitochondria for the formation of ATP and plenty of blood supply for a continuous supply of nutrients & oxygen in cardiac muscle. |
| But in the skeletal muscle, there is not plenty of mitochondria & blood vessels. |
| Excessive exercise causes a lack of oxygen leading to the formation of lactic acid from anaerobic glycolysis, which makes fatigue. |
| Lactic acid formation doesn’t occur in cardiac muscle due to the large number of blood vessels providing adequate oxygen supply. So, no anaerobic process occurs. |
| • Bursa is required when a tendon or bone experiences friction on one surface only. |
| • Mostly found around the synovial joint. |
| • When a tendon glides over a bone or ligament, bursa appears to diminish the friction & to allow free movement. |
|
• Normally in non-excitable conditions, inside of the membrane is in the polarized state
That means more -ve charge than outside.
|
|
• Depolarization:
Polarized (-ve) stage inside the membrane is turned to +ve depolarized stage due to the rapid influx of +vely charged Na+ ions.
|
| • The electrical potential difference on the two sides of the cell membrane at the resting stage is called Resting Membrane Potential (RPM). |
| • Action potential means rapid change in RMP from normal (-ve) value to (+ve) direction & again return back to normal (-ve)potentials. |
| • Motor end-plate: The thickening portion of muscle fiber nearest to the invagination of the motor neuron terminal into the muscle fiber. |
| The propagated action potential is called impulse. |
| Neuromuscular junction: Synaptic Junction between motor nerve ending & Skeletal muscle fibers. |
| Within Synaptic vesicles - contain neurotransmitter (acetylcholine) |
|
Generation of action potential in the neuromuscular junction (Neuromuscular transmission)
↓
When motor impulses travel along the motor nerve terminal
↓
Open voltage-gated Ca++ channel
↓
Ca++ enter into the vesicles present in the motor nerve terminal
↓
Causes releases of acetylcholine(neurotransmitters) then diffuses toward synaptic cleft and bind with the receptor protein of motor nerve end plate
↓
Increase permeability of Na+ and causes depolarization of the membrane.
↓
When enough Na+ accumulated, causes enough depolarization causing generation of action potential
↓
Action potential then travels along T Tubules.
|
|
Discharge of impulse in motor neuron
↓
Release of neurotransmitters (acetylcholine) at the motor end-plate
↓
Binding of Acetylcholine to Nicotinic Acetylcholine receptor
↓
Increased permeability of Na+ inside the motor end-plate membrane
↓
Enough depolarization causes the generation of the action potential in muscle fibers
↓
Inward spread of action potential along T tubules
↓
Release of Ca++ from terminal cisterns of sarcoplasmic reticulum into sarcoplasm(cytoplasm)
↓
Binding of Ca++ to Troponin C (protein) present in thin actin filament
↓
Formation of cross-linkages between thin actin & thick myosin filaments
↓
Sliding of thin on thick filaments producing shortening/ contraction movements
|
|
When action potential stops
↓
Ca++ pumped back into the sarcoplasmic reticulum
↓
Release of Ca++ bonded to Troponin C
↓
Cessation (stop) of interaction between actin & myosin
|
|
Action potential along T-tubules
|
Ca++ released from the terminal cisternae of sarcoplasmic reticulum
|
Ca++ ions bind with troponin C
|
Inhibition of troponin-tropomyosin complex
|
Uncovers the active site of the actin
|
Interaction of actin & myosin
|
Muscle contraction
|
| This Development of skeletal muscle might help in understanding how the single skeletal muscle fiber, an example of true syncytium. |
| All muscles develop from mesoderm except muscles of iris & Arrectores pilorum (Muscle of the skin) & (Myoepithelial cells of salivary, sweat & lacrimal gland) which are ectodermal in origin. |
| Nerve & muscle are called excitable tissue because they are capable of generating rapidly changing electrochemical impulses of their membrane. |
Comments (0)