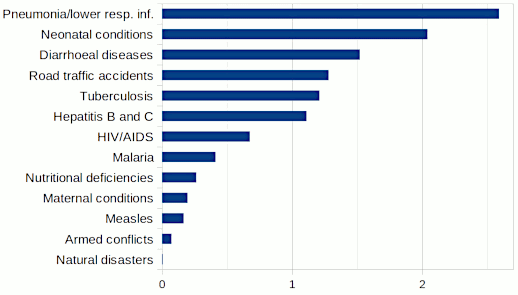
Methods for Generating Health Estimates
In the process of producing health estimates, there are a number of different factors that need to be considered. The first step is to define the problem and how to measure it. This should include the methods used, as well as the covariates and guidelines for reporting. There are several methods that are available to health practitioners and researchers. For example, indirect methods are based on demographic techniques, rather than primary or secondary sources of information. This method is often more accurate but can have issues with data sources that do not exist. Population counts and core indicators of life events can also be affected by the absence of data.
Cost of health care
To calculate the total cost of health care, you must understand how healthcare resources and processes are used in a health system. In this case, Patient Jones makes an outpatient visit to the clinic. She uses administrative processes such as check-in, registration, and third-party reimbursement, and clinical processes such as treatment. The costs for each process include resources used to ensure the patient's safety, comfort, and satisfaction. The following table shows the costs of these processes, along with their associated resources.
The costs are often not accurate and are often based on arbitrary assumptions about the intensity of care. In addition, the costs are often very high if patients have to pay high copayments. This limits their ability to use expensive drugs, which leads to ballooning costs elsewhere in the system. Additionally, a patient's overall health can deteriorate, requiring more services. Ultimately, the cost of health care is an inexorable problem for many health systems and their patients.
Methods
Health indicators are increasingly needed to monitor progress towards global and regional goals. They can also inform the allocation of resources and policies. The methods of generating health estimates are often complex and highly dependent on the input data and the underlying analytic assumptions. In addition to this, they are difficult to explain to non-experts. Therefore, it is essential to describe the methods of health estimate generation in detail. This article aims to explain the basic principles that must be adhered to when developing health indicators.
Health indicators are derived from the results of studies that synthesize data from different sources. Some of these studies provide estimates for a particular time period or geographic area. These articles report the health status of individuals and populations and the health determinants of the populations. The methods used in these studies are often incomplete, but the guidelines outlined in the GATHER are meant to improve the quality and reliability of health estimates. This will make them more accessible to the public and help to improve their credibility.
Covariates
When assessing the effectiveness of Health Estimates, a study's statistical analysis should consider covariates in its design. For example, an adjustment of the propensity score for a given treatment group may reduce its effectiveness. A time-varying covariate may be a confounder and alter an outcome. Moreover, it may be the only relevant predictor of the effect of a particular treatment. The choice of the covariate-balancing method should take this into consideration.
A time-varying confounder may affect the outcome differently in two studies that are similar in age and gender. In these cases, adjusting for time-varying confounders is crucial to produce unbiased estimates with an optimal SE. Time-varying confounders can affect a study's results and violate the causal assumptions underlying the study. Regardless of whether or not a study uses time-varying confounders, it is important to consider how the inclusion of these factors affects its overall results.
Guidelines for reporting
Currently, a standard used by health care providers to report health estimates is the GBD (Guidelines for reporting health estimates). It is an acronym that stands for "Guidelines for the reporting of accurate and transparent health estimates". It is designed to prevent errors in health care reports and ensure that the data reported are as accurate and transparent as possible. However, there are a number of limitations to this standard. The following are some examples of the limitations of the GBD.

Comments (0)